Orthopaedic Knee Review
The Knee - a review of current practice
Information written by Tim Spalding
Updated by Adam Pearce, 3rd Year Medical Student
- Acute knee injuries: Diagnosing the Torn ACL in the Acute Knee
- Osteoarthritis of the Knee and Knee Replacement
- Meniscal Injuries
- Patello-Femoral Problems
Appendix A – Arthroscopy of the Knee
Appendix B – Obesity and the Knee

6th Edition -February 2015
Contents
- Orthopaedic Knee Review
- Appendix A – Arthroscopy of the Knee
- Appendix B – Obesity and the Knee
- Diagnosing the Torn ACL in the Acute Knee
- Osteoarthritis of the Knee
- Meniscal Injuries
- Patello-Femoral Problems
Orthopaedic Knee Review
The Knee - a review of current practice
Information written by Tim Spalding
Updated by Adam Pearce, 3rd Year Medical Student
- Acute knee injuries: Diagnosing the Torn ACL in the Acute Knee
- Osteoarthritis of the Knee and Knee Replacement
- Meniscal Injuries
- Patello-Femoral Problems
Appendix A – Arthroscopy of the Knee
Appendix B – Obesity and the Knee

6th Edition -February 2015
Contents
Appendix A – Arthroscopy of the Knee
Introduction
Arthroscopy of the knee is an operation in which a small camera, and possibly surgical instruments, are inserted into the knee through two or three small puncture wounds. Understanding what the basic procedure entails is straightforward if we look at the etymology of the word.
- arthro- : relating to joints
- scopy: viewing, observation or examination
Arthroscopic procedures have equivalents in other branches of surgery. Examples include laparoscopy (laparo-: of the abdominal wall) in general surgery and cystoscopy (cysto-: relating to the urinary bladder) in urology.
Arthroscopic procedures
In the most basic of arthroscopic procedures, the structures within the knee are viewed and assessed using a camera called an arthroscope, with a view to diagnosis. The structures examined include the meniscus, the synovium, the articular cartilage and the cruciate ligaments.
Depending on findings, additional therapeutic procedures can be carried out via the insertion of surgical instruments. Such procedures include:
- Debridement: Particularly in patients with mechanical symptoms such as locking, debridement can be helpful by removing a torn piece of meniscus – in which case the procedure is called an arthroscopic meniscectomy – or other tissue. Rough, damaged articular cartilage can also be treated in this way.
- Mensical repair: In certain cases, repair of a torn meniscus can yield better results than mensisectomy.
- Loose Body Removal: Some injuries can cause fragments of bone, cartilage or other soft tissues to break off within the knee. These can be found and removed arthroscopically.
A first guide to interpreting arthroscopic images
Many patients seen on the ward and in clinics will have arthroscopy reports and associated images in their notes. For medical students, junior doctors and the patients themselves, these images can sometimes be disorientating, as it is necessary to imagine you are inside the knee to work out what the different structures are. Here, a few simple rules for orienting oneself to the images are presented.
- Rule 1: Ensure you determine which knee you are supposed to be looking at. This simple step is key to understanding which side of the image is lateral and is which is medial.
- Rule 2: Most of the images are taken looking antero-posteriorly – i.e. from the front of the knee towards the back. The exception to this rule is those images taken looking upwards at the patella-femoral joint.
- Rule 3: The surgeon handling the arthroscope will keep the tibial plateaus horizontal and towards the bottom of the image whenever they can be seen.
- Rule 4: The surgeon will have manipulated the knee to open up the joint space in the area where each image is being taken. This can give a false impression of the spatial relationship between the articular surfaces and the soft tissues.
The images below, of a left knee joint, are annotated with reference to the rules above, to clarify which part of the joint they show.

This is the inside of a left knee, viewed from the front. Any structures on the left of the page are therefore on the medial side of the knee, and those on the right are lateral.

The tibial plateaus are kept horizontal at the bottom of the image.
The medial meniscus is shown ‘floating’ between the two articular surfaces. Under normal load, the meniscus would be compressed between the two.
This is the inside of a left knee, viewed from the front. Any structures on the left of the page are therefore on the medial side of the knee, and those on the right are lateral.
The tibia plateaus are kept horizontal at the bottom of the image.
In this case, we can see a defect in the articular cartilage of the lateral tibial plateau, as indicated by the probe.

Again, this is the inside of a left knee, this time viewed looking upwards at the patella-femoral joint. Lateral and medial are the same as the images above.
The key to understanding the orientation of this image is to recognise the wedge-shaped posterior surface of the patella and the trochea groove of the femoral condyles.
In this case, the articular surfaces to the bottom of the image are the femoral condyles.
Appendix B – Obesity and the Knee
Introduction
Obesity is one of the most common comorbidities in patients seen in the knee clinic. With obesity levels in the UK rising every year, over 50% of the population is set to be clinically obese by 2050. At such levels, it is projected that Obesity could cost the NHS nearly £50 billion per year.
The mechanical implications of obesity for the knee and other joints in the body are, perhaps, obvious. However, overloading is not the only way that obesity can affect the knee. The full range of issues associated with obesity can be grouped as follows:
- Mechanical factors
- Systemic factors
- Surgical factors
- Anaesthetic factors
Each of these areas is discussed briefly, below.
Mechanical Factors
The most recognised and well-studied association between obesity and knee pathology is that of osteoarthritis. Obese patients place increased stresses on their articular cartilage, which drives earlier onset and more rapid degenerative changes. Furthermore, there is a higher rate of varus alignment in the obese population, which places additional stress on the medial compartment of the knee joint.
Apart from osteoarthritis, a recent study has shown that obese patients are more likely to suffer multi-ligamentous knee injuries due to low energy mechanisms. Such injuries can be devastating for the function of the knee, particularly when considering the difficulties associated with surgery and obesity, which are discussed below.
Systemic factors
Overloading alone does not account for all of the increased morbidity associated with osteoarthritis in the obese population. Over recent years, it has become increasingly evident that adipose tissue has a role as an endocrine organ, producing a variety of hormones and biochemical factors that affect the function of a wide variety of systems in the body. Many of these chemicals – including chemokines, cytokines and adipokines – are pro-inflammatory and therefore exacerbate symptoms such as pain and swelling associated with arthritis. They are also thought to disrupt the delicate balance of anabolic and catabolic processes within joints, which can lead to increased degeneration of cartilage and other soft tissues. The role of adipose tissue helps explain why osteoarthritis of non load-bearing joints – e.g. in the hands and fingers – is also more common in obese patients.
Surgical factors
There are a number of ways in which obesity affects surgical procedures and outcomes. It should come as no surprise that procedure time is increased for obese patients, as is the overall length of stay in hospital. Obese patients are also likely to experience worse overall outcomes and satisfaction levels following their operation. For example, in total knee replacement surgery for normal weight population, around 90% of patients will be satisfied with the result. In the obese population, only 70% have a good outcome. At least part of the reason for this is increased rate of complications, such as delayed wound healing, more post-operative pain and increased rates of deep vein thrombosis.
Anaesthetic factors
In general, obesity is a risk factor for a number of systemic diseases, such as cardio-respiratory (eg. hypertension, heart failure), metabolic (eg. diabetes) and gastrointestinal conditions (eg. gastro-oesophageal reflux disease), all of which can have anaesthetic implications.
Specific difficulties that the anaesthetist may encounter include:
- airway problems associated with anatomical restrictions and sleep apnoea, which can also cause perioperative drowsiness, complicating assessment and treatment.
- Ventilation problems due to difficulty intubating the patient, reduced lung capacities and low chest wall compliance.
- Inaccurate blood pressure readings using normally available cuff sizes
- Unpredictable pharmacokinetics leading to unknown rates of drug elimination, etc.
- Loss of landmarks for regional anaesthesia
- More difficult venous access
The Good News
For the reasons outlined above, obese patients can experience dramatic improvements in their symptoms and response to treatment if they are able to lose weight. The effects of mechanical, systemic and other factors are additive, such that even a reduction of a few percent (5% – 10% is often targeted) can deliver significant benefits. The systemic effect of adipose tissue means that greater benefit is derived if weight loss can be achieved through reduction of body fat percentage, rather than loss of muscle. Studies have shown that good advice alone is not sufficient for successful weight loss – patients who are actively supported through the process tend to do much better. In cases of extreme obesity, patients may wish to consider other weight—loss options, such as bariatric surgery, before electing for orthopaedic surgery.
Diagnosing the Torn ACL in the Acute Knee
Introduction
When dealing with the acutely injured knee, the detection of injury to the anterior cruciate ligament (ACL) is an essential part of the management aim. Most acute knee injuries will settle over time and patients will be tempted to return to sport. However, ruptures to the anterior cruciate ligament will result in a patient feeling perfectly stable on their knee while running in straight lines but they will be at risk of their knee giving way again if they try to pivot or twist on it. Subsequent episodes of giving way are likely to result in a tear to the meniscus (footballer’s cartilage) or damage to the articular cartilage. This second injury starts the downward spiral towards later degeneration in the knee.
It is for this reason that this section directs diagnosis towards excluding rupture of the anterior cruciate ligament.
Anatomy and Function of the ACL
The anterior cruciate ligament acts as the main link mechanism between the tibia and the femur, preventing anterior movement of the tibia on the femur. When pivoting therefore, the femur and tibia usually act as one but without the ACL the tibia is allowed to jump forward and back again creating the sensation of the knee giving way.
Differential Diagnosis
Injury to the ACL is, of course, only one of the potential diagnoses that need to be considered in the acutely injured knee. Others include:
- Meniscal tear
- Collateral ligament tear
- Patella dislocation
- Ruptured posterior cruciate ligament
- Simple knee sprain
The key features of each of these injuries are described below.
a. ACL rupture.
The mechanism of injury is usually a non-contact situation associated with rapid deceleration. The patient may describe a pop or a snapping sound and they are usually unable to play on. If they do then the knee gives way again. Swelling appears within four hours or so and diagnosis is made on the Lachman and pivot shift test.
b. Torn meniscus.
The mechanism to tear the meniscus is usually a weight bearing twisting injury, often associated with a tearing sensation. The knee may be locked as the meniscus obstructs full extension of the joint. Swelling appears more delayed than after ACL rupture, often after four hours and usually overnight. Diagnosis is made by eliciting tenderness on the joint line.
c. Collateral ligament injury.
The mechanism for injury to the lateral collateral ligament or medial collateral ligament is a blow from the side of the knee resulting in localised pain on the attachment points to the ligament with tenderness over the affected femoral condyle. Swelling is variable and is usually outside of the joint.
d. Patella dislocation.
Patella dislocation is often difficult to elicit and it depends on the history from the patient who may describe a sensation of their knee dislocating. This often has to be specifically asked for. Tenderness is usually felt around the medial para-patella border, immediately adjacent to the patella. The patient would be reluctant to allow their patella to be pushed laterally.
e. Posterior cruciate ligament.
The PCL is injured by a direct blow to the anterior part of the tibia driving the tibia posteriorly or by a significant hyperextension mechanism. The symptoms will be variable but the main sign is posterior sag of the tibia on the femur when viewed from the side (sag sign).
Diagnosis of ACL Deficiency
Diagnosis in the acute setting is made by the history of mechanism and specific findings on examination. In the patient who complains of repeating episodes of giving way then there will often be found a history of an injury some months or years before associated with a significant downtime from sport and a persistent feeling of not trusting the knee on pivoting and turning.
The main signs on examination are the positive Lachman’s test and pivot shift test, each described briefly below. See the document ‘History and Examination of the Knee’, available on www.timspalding.com, for more in-depth information regarding clinical assessment of the knee.
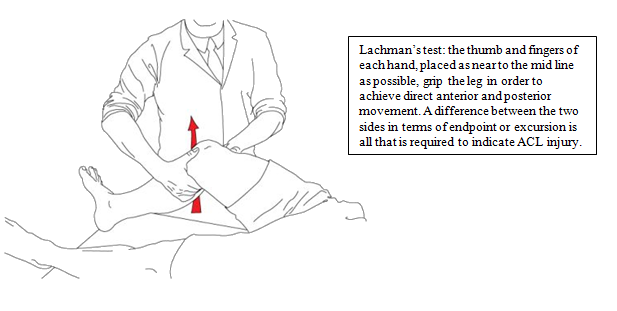
In the Lachman’s test the knee is held at 15° flexion and an anterior drawer made on the tibia against the femur sensing increased movement.
The pivot shift test is diagnostic of ACL rupture as it reproduces the patient’s sensation of the tibia jumping on the femur.
Management Principles
The main principle for managing the acute knee is to attempt to assess the knee in the acute setting and then to immobilise the joint with a supportive bandage or splint for 2 or 3 days prior to further examination.
Ice may be applied to try and reduce pain and swelling. Aspiration for analgesia is generally reserved for the severely tense knee which is very painful due to the tension. Such a knee may benefit from removing the bleeding from the joint.
After a few days rest mobilisation is attempted aiming for gradual increase in range of movement while re-evaluating the knee at various time intervals over the subsequent six weeks.
This management plan is based on the principle that most minor injuries will settle by six weeks and that some meniscal tears can heal without needing urgent intervention.
URGENT REFERAL TO HOSPITAL: The main indication for referral to hospital acutely is for a locked knee (where the leg will not go fully straight) and the very unstable knee where there is possibly complete rupture of the medial collateral ligament.
ACL Management Plan
Management of the sportsman with rupture to the anterior cruciate ligament is based on multiple factors. The principle is early diagnosis in order to prevent the second episode of giving way that may subsequently damage the meniscus or articular surface. Early rehabilitation following injury is directed at regaining full range of movement, balance control and re-learning confidence in the knee.
A decision is made on the level of sporting aims and, if considered appropriate, then reconstruction surgery is performed after the acute inflammation has settled. This is usually at six to twelve weeks post injury allowing a return to contact sport at six to nine months.
Joint Surface Damage
We know that the time interval between injury and reconstruction increases the risk of articular cartilage damage and this knowledge argues in favour of early reconstruction of the anterior cruciate ligament before any repeated episodes of giving way have caused damage to the joint surface.
The area of articular surface damage is related to the time since injury and also to the state of the meniscus. The area is increased six fold if it is more than two years since injury and three fold if associated with loss of the meniscus.
Ten years following ACL rupture the incidence of degenerative change seen on the x-ray is only 10% in the presence of a normal meniscus but is up to 60% if the whole meniscus has been removed.
Surgical Reconstruction of ACL Injury
ACL reconstruction is now a reliable procedure with over 9 out of 10 reconstructions resulting in a normal or nearly normal knee. The aim of reconstruction is to improve function and it is not appropriate to say that reconstruction actually prevents arthritis in the long term. It is known that arthritis following the ACL is related to the secondary injury and has a higher prevalence where the meniscus or articular cartilage has been damaged.
Repeated giving way of the knee results in increased chance of injury to the meniscus and to shear injury on the articular surface. There is a 45% chance of tearing the meniscus over a three to five year period if an individual continues to play sport with an unstable knee.
The best results from ACL reconstruction are seen when there has been no previous tear to the meniscus or damage to the articular surface.
Surgical Techniques
Currently the surgical technique involves reconstituting the cruciate ligaments using the hamstrings (semi tendinosis and gracilis tendons) harvested through a small incision. The newest techniques focus on inserting the graft in the true anatomical position and recent work at UHCW and published in the Journal of Arthroscopy has helped improve the accuracy of the surgery.
Occasionally the central third of the patella tendon (10mm wide strip of the patella tendon with bone from the patella and tibial tubercle) is used for the graft
In the operation the new tissue is fashioned into an appropriate size and tunnels are drilled into the femur and then through the tibia and the operation is assisted by use of the arthroscope. For information on other arthroscopic procedures, see Appendix A.
The new graft is held in placed using either a metal ‘endobutton’ device on the femur and a tensioner system with absorbable screw on the tibial side. When the Patella tendon graft is used this is held in place with bioabsorbable screws.
Post Operative Rehabilitation
Following ACL reconstruction patients are discharged home on the day following surgery, walking with two crutches with their leg in a light tubigrip support. No braces are used.
Patient should expect to have a comfortable 90° bend by two weeks and to be back to activities of daily living by four weeks.
Driving is allowed at three to four weeks and this is often the time for return to deskwork.
Standing work is usually tolerated after six weeks whereas heavy manual work is generally not expected for three months. Return to scaffolding, ladders or roof work is expected at four months.
As regards return to sport, running is started at two to three months but pivoting is not allowed for four months. Contact sport training is commenced at six months and patients could usually be back to full sporting activity at around nine months.
Summary
When faced with the acutely injured knee, our aim is to repeatedly assess the knee with a view to making an early diagnosis of rupture of the anterior cruciate ligament. The principle is to try and prevent repeated giving way and it may take repeated examination to detect any laxity and looseness in the knee. Patients should be referred for specialist opinion via A&E early if there is an acutely locked knee or significant ligament laxity is detected.
If symptoms do not settle over the first six weeks then patients should be referred before they recommence sport, so that rupture of the ACL may be confidently excluded.
ACL reconstruction is now a procedure with greater than 90% success and late diagnosis of ACL injury is associated with a worse outcome.
Osteoarthritis of the Knee
Introduction
Total knee replacement (TKR) has now become a very common and successful procedure for managing the severely arthritic knee. Pain relief is generally excellent and the level of function that a patient can expect is improving with advances in both the surgical technique and in rehabilitation.
This means that knee replacement is being offered earlier in the process of deterioration of knee function associated with osteoarthritis and the aim of this chapter is to describe the place and indications for TKR in the management of knee OA.
It is important to remember however that knee replacement is the end stage of a long ladder of treatment options available for the management of early, mild and moderate knee osteoarthritis.
Symptoms of Knee OA
The main symptoms are pain, swelling, and stiffening in the knee. Symptoms tend to develop slowly over several years and are generally activity-related. Symptoms tend to be noticed after keeping the knee still for prolonged periods, only to be relieved by exercise but being made worse after too much activity. Often there is a history of repeated flare-ups with quiescent periods in between. Eventually, symptoms tend to affect sleep patterns.
Signs of Knee OA
The main signs are swelling, broadening of the knee joint and deformity. Diagnosis is generally made more on history than on the signs. A more in-depth account of history and examination of the knee is considered in the document ‘History and Examination of the Knee’, which is available for download at ww.timspalding.com.
Radiographs can be used to quantify the extent of the wear but are generally used to rule out other problems.
Non-Surgical Treatment Options
The mainstay of treatment for knee osteoarthritis is to improve the symptoms as it is generally not possible to alter the underlying disease process. As mentioned above, surgical treatment of knee osteoarthritis – in the form of Knee Replacement – is the end of a long ladder of treatment options. The following are all important in the management of knee OA, and are briefly described in turn, below.
Conservative Treatment
a) Activity and lifestyle modification
b) Physiotherapy.
c) Unloading type knee braces.
d) Walking aids
Medical Treatment
e) Analgesic and anti-inflammatory medications.
f) Nutritional Supplements, such as Glucosamine or Chondroitin
Injections into the Knee
g) Viscosupplementation injections.
h) Steroid Injections
a) Activity and Lifestyle Modification
Certain low-impact activities such as swimming, cycling and walking are excellent for building muscle, which then helps to support the knee and other joints of the body, preventing the unstable loading that can cause pain and further degenerative changes. Physical activities can also help reduce body weight, which further reduces load on the knee. Nutritional aspects are also very important in this context, and a balanced diet has numerous benefits for joint and general health.
b) Physiotherapy
Improvement in muscle control, balance, flexibility, strength, and gait can all help to unravel any detrimental effects of weakness or imbalance on loading of articular cartilage of the joint. The physiotherapist aims to ensure that forces are distributed evenly across the joint by assessing the patient holistically. The spine, hips, knees, ankles and feet can all impact on the forces transmitted through the knees, and should all be assessed.
c) Unloading Type Knee Braces
These braces are worn around the leg. They are called ‘unloading’ type because they unload a damaged area of the joint surface and redistribute the forces to another area. For this reason, they are particularly helpful for patients suffering from unicompartmental symptoms, such as those who have varus deformities of the knee.
d) Walking aids
Walking aids, such as sticks and canes, can be helpful for those whose symptoms limit their functional abilities. Uneven ground, for example, may present a particular problem to somebody with poor muscular control of the joint. In this situation, a cane to add stability when walking on the uneven surface could be considered.
e) Analgesic and anti-inflammatory medications
Painkillers taken orally – such as Paracetamol – or applied topically – such as Capsaicin, can be very effective at controlling the pain associated with osteoarthritis. Some patients express concern that taking painkillers is simply masking the underlying cause of their problems. Careful explanation of the benefits of symptom control and the fact that analgesia forms a valid part of the treatment ladder may therefore be necessary. Anti-inflammatory medications such as ibuprofen can also be taken orally or applied topically.
f) Nutritional Supplements
Sometimes referred to as ‘neutraceuticals’, these products are not classified as medications but have the potential to provide physical benefits. Two of the most commonly taken supplements are Glucosamine and Chondroitin, and they are often taken together. Both naturally occur within the body and are key components in the production of extracellular matrix (ECM). It is therefore thought that supplementation with these products can help delay degenerative connective tissue changes. There is some disagreement within the research community regarding the degree of benefit that can be derived, but the relief of moderate to severe joint pain has been shown at high doses (1500 mg/day for Glucosamine, 800-1200 mg/day for Chondroitin). Given their low side effect profiles and relative inexpense, they have a deserved place alongside or instead of other therapeutic options.
g) Viscosupplementation injections
Viscosupplementation injections in the knee, such as Synvisc One, have shown promise in affecting symptoms. We have found that 50% of patients with mild to moderate arthritis show an improvement in their symptoms after Synvisc injections. This lasts for up to nine months. The active ingredient in the injections is hyaluronic acid or hyaluronan. It is thought to work both mechanically, by acting as a viscous lubricant of the articular surface – and therefore decreasing the coefficient of friction – and biochemically via its anti-inflammatory properties. Synvisc One is a single injection and Ostenil involves a course of 3 injections with a week’s gap.
h) Steroid Injections
Corticosteroids have anti-inflammatory properties and can therefore be helpful in controlling acute flare-ups of osteoarthritis. They are often combined with a local anesthetic to reduce the discomfort of the injection itself. The local anesthetic will start to work within a few minutes, but will not generally last longer than around half an hour. The anti-inflammatory effect of the steroid generally starts within a few hours to a few days of the injection – depending on the specific corticosteroid used – and lasts between four to eight weeks.
Surgical Options
The variety of surgical options includes:
a) Arthroscopy
b) Osteotomy – high tibial or distal femoral
c) Partial resurfacing
d) Isolated patello femoral arthroplasty.
e) Uni-compartmental knee replacement.
f) Total knee replacement.
a) Arthroscopy
Arthroscopy at its most simple involves looking inside the knee by inserting a camera through a small incision. There are a variety of interventions that can subsequently be carried out during the same procedure, based on the findings. These are considered in more detail in Appendix A. In the context of the degenerative changes seen in osteoarthritis, arthroscopic techniques can be used in the treatment of degenerative tears, tight adhesions, unstable flaps of articular cartilage and removal of inflamed synovium.
b) High tibial or distal femoral osteotomy
Osteotomy is performed to re-align the leg where there is mal alignment and arthritis developing in the overloaded medial or lateral compartment. Two types are generally undertaken – high tibial, which is the most common and is used to correct a varus (“bow leg”) deformity, and distal femoral, which is used to correct a valgus (“knock-kneed”) deformity. Not all legs need to be corrected as these alignments can be physiological. However if there has been an injury to the knee and part of the meniscus has been removed then the joint is prone to rapid deterioration.
The main indication is for early wear and tear affecting the varus or valgus knee in the under fifty year old. It is best done before the joint surface is completely worn down to bare bone but this is often the phase where patient has less symptoms and does not relish the prospect of two months on crutches and possibly up to four to six months getting back to outdoor activities.
However, in the right patient the concept of “buying time” and slowing down the wear process is appropriate and in general, as a rule of thumb, for isolated medial or lateral degeneration osteotomy would be advised for the under 50 year old to preserve their own joint as long as possible, and arthroplasty would be indicated for the over 60 year old with sufficient symptoms.
For patients between aged 50 and 60 a decision is made based on level of symptoms, intended lifestyle, occupation, hobbies and patient plus surgeon preferences.
Managing the athletically active arthritic knee remains an interesting challenge and so far we have over 150 osteotomy patients in our database.
c) Partial resurfacing
If only a very small area of articular cartilage is damaged, it may be possible to avoid removal of all or half of the joint surface with metal and plastic. Two new partial resurfacing options are available. The smallest – called Hemicap – is a metal implant that fills in an area of articular cartilage damage on the femur. The manufacturer likens their product to a filling for a tooth. The healthy surrounding cartilage remains in place. A slightly larger component – a Unicap – is also available. This involves resurfacing both the femur and the tibia. Both of these can be useful options for younger patients who wish to avoid – or at least delay – the need for a partial or total knee replacement. It can also be used in those who have suffered focal chondral damage as a result of trauma.
d) Isolated patello-femoral arthroplasty
Arthritis that is localised to the anterior compartment of the knee – the patella-femoral joint – can occur. It is particularly common in women, as a result of minor mis-alignment and maltracking that is more common in females. Whilst total knee replacement will predictably remove any pain associated with this condition, it is an undesirable choice for many younger, active, patients. For this reason, isolated patella-femoral arthroplasty is proving to be a very good alternative for management. The procedure involves resurfacing the patella with a plastic button and the articulating femur surface with a metal conforming implant. The procedure is now very popular, with good results reported.
e) Unicompartmental knee replacement
Uni-compartmental knee replacement involves resurfacing usually the medial part of the joint (femur and tibial surfaces). It is possible to resurface the lateral part but this is a much less common procedure.
Surgery is performed through a small incision, about 10cm long and as such hospital stay is about 3 – 4 days.
To undertake this surgery the arthritis has to be limited to the medial compartment and there should be no significant patella-femoral symptoms. Also, the ACL needs to be intact for the mechanism to work.
The long term results are as good as total knee replacement but it can still take two to three months to fully get over. It is usually much more comfortable in the early phase and this, combined with the short hospital stay, makes it a very appealing option for the appropriate patient.
f) Total knee replacement.
The indications for knee replacement are symptoms of:
• Pain
• Loss of function.
• Abnormal movement.
These symptoms are, of course, all relative and the level of symptoms which will justify the risks for undergoing knee replacement have evolved over recent years.
Each decision is based on balancing the following factors.
1. Pain.
This is the main factor. Pain should be poorly controlled by analgesics or anti-inflammatory medication. There should be night pain and difficulty in getting to sleep because of knee pain.
2. Loss of Function.
Loss of function without pain is not an indication for knee replacement. Loss of function is usually associated with pain and the level of restriction that is considered to justify knee replacement is a walking tolerance of less than a mile, difficulty climbing stairs and a feeling that ‘life is on hold’ due the knee symptoms.
3. Abnormal Movement.
Severely varus or valgus knees or knees with significant instability may mean that knee replacement is employed earlier rather than waiting for further deformity.
4. Age.
The life span of the knee replacement implant is unfortunately limited and therefore the intention of surgery is for the implant life span to extend beyond the life span of the individual without revision. In individuals aged over sixty one can expect a 95% ten year survival of the knee replacement extending to 90% at fifteen years and 85% at twenty years.
In individuals under age sixty one can only expect that 70% of knee replacements will still be satisfactory after ten years.
To summarise, over age 60 we would expect one knee replacement to see the patient out whereas under age 60 a patient should expect revision. The results of revision surgery are far less predictable.
5. Obesity.
Obesity is not a contraindication to knee replacement. There is no clear effect on survival rates and it has been shown on various occasions that the relative benefit of knee replacement in the obese patient is greater. Obesity is a very important topic in orthopaedics, and its relevance to the knee is considered in more detail in Appendix B.
6. Expectations.
This is perhaps the second most important factor after the level of pain. It is hard to define expectations but the following phrases summarise the issues:
• Total knee replacement gives you the knee function of a 70 year old not a 20 year old.
• With a knee replacement you can walk five miles and perhaps play light doubles tennis, provided you can say ‘yours’ and ‘nice shot’.
• It is a metal and plastic knee that does not feel like a normal knee.
• Nine out of ten go extremely well but one in ten can have severe problems after surgery making you potentially worse off.
• Mild pain is normal after knee replacement and 10 – 15% of patients can have persistent moderate pain at one to two years.
Post Operative Recovery
Since the introduction of the technique of Mini-Incision knee replacement in November 2003 and, more recently, an enhanced care program, the length of recovery in hospital has been substantially shortened such that we aim for most patients to go home on the 4th day after surgery. This is nearly half the previous length of stay. In the technique the patella is slid to the side rather than everted which traditionally required a longer cut in the quadriceps tendon. The usual incision length is now 12 – 14 cm compared with 18cm before.
Much of the progress toward earlier recovery and discharge home has been made in the better control of the discomfort after surgery and the earlier mobilisation. On discharge patients should expect to be able to cope with stairs and should be using crutches or sticks. It is usual to progress onto one stick easily by the six week stage and to discard support after the six to eight week outpatient review.
Patients are advised that it generally takes up to three months to get over a knee replacement and this usually equates with return of good function and a feeling that the swelling has gone down with the re-emergence of a normal contour to the knee.
Warmth in the knee however usually persists for up to six months and is not a cause for concern. Reassurance is sometimes required.
Patients will often say that their knee felt better even at a year following surgery but there is generally little change after that stage.
Range of Movement
The average range of movement achieved after knee replacement, according to our recent analysis, is 106° . A lot of patients therefore are achieving greater than this range and this has a substantial bearing on knee function. It is possible to achieve full range of movement (heel to buttock) but this is usually dependant on the amount of bend in the knee that was present prior to surgery. Achieving this range, in turn, is very much dependant on the efforts of the patient adhering to the rehabilitation programme.
In functional terms, a knee that only bends to 90° means that the patient has to push up on the arms of the chair in order to stand. Bend beyond the 100° allows the patient to tuck their heels behind themselves, under the chair, and stand up easily. We are generally unhappy therefore if the patient has only achieved 90° !
Meniscal Injuries
Introduction
The meniscus, or footballer’s cartilage, is the protective shim between the femur and tibia. It is classically injured in a weight bearing twisting type mechanism.
The main function of the meniscus is to protect the articulating surfaces of the bone by distributing the load across the joint. The lateral meniscus is the most important as it takes 70% of the weight that goes through the lateral half of the joint. Removal of this structure therefore results in a dramatic increase in load through the joint and early failure of the articular surface.
The articular cartilage is the smooth glistening white surface that is virtually frictionless. Damage to this surface results in increased friction and wear on the joint. This leads to further damage and degeneration – osteoarthritis.
Diagnosis of a torn meniscus
A full house of symptoms and signs for a diagnosis of a torn meniscus are as follows:
- History of weight bearing twisting injury.
- Effusion in the knee joint.
- Specific joint line tenderness.
1. Injury Mechanism.
Injury to the meniscus can occur in virtually all age groups and the underlying theme is a twisting injury on the weight-bearing knee. In the younger active individual tears tend to be classified as traumatic in pattern where there is a clean tear through a healthy meniscus. The opposite pattern is a “degenerate” style tear with much more of an irregular crushed appearance. Such tears often exist in the generally degenerate knee.
2. Effusion.
The torn meniscus irritates the joint generating an increase in synovial fluid forming an effusion. This is seen as a swelling in the medial, lateral and supra patella area. The patient may describe this as ballooning of the joint or loss of the normal divot or dent seen on the medial aspect of the patella. With time the swelling will settle only to recur after a minor twisting injury. Patients may therefore avoid going back to activity for fear of re-inflaming the knee.
3. Joint line tenderness.
This is very specific to a meniscal tear and there is a pinpoint location on the medial or lateral side associated with the relevant injury (see diagram) To find this area the joint line has to be identified and this is best found by initially palpating the soft spot on either side of the patella tendon and following the soft line posteriorly from that point between the femur and the tibia. It is best felt by firmly applying the pulp of two fingers to the joint line and slightly rubbing in a superior / inferior direction to generate point tenderness. This can be compared to the other knee if there is doubt as to whether there is genuine tenderness compared to normal. The tender point on the medial side is slightly more posterior than on the lateral side.
Lateral meniscal tears may be associated with a swelling or cyst formation which is a fullness felt on the joint line overlying the mid part of the lateral meniscus.
The knee joint may often need to be supported with the other hand in order to generate sufficient pressure to elucidate the tenderness.
Symptoms
The main symptom of a torn meniscus is pain and this is generally well localised to the edge of the knee joint. If there is significant swelling in the joint then this will manifest as a sensation of stiffness and tightness on bending the knee.
A further symptom is intermittent locking or giving way as the torn fragment of meniscus catches. By a locking we traditionally mean that the knee will not go fully straight as the torn fragment blocks the space between femur and tibia preventing full extension.
Treatment Options and Timing
Not all meniscal tears need surgical treatment and acute tears need time to be allowed to heal on their own. In general a tear that settles down and does not cause swelling in the knee does not need operative treatment if it is not causing significant pain or interference with function.
In the acute setting some tears can heal and if this is to happen then it is usually clear by six weeks whether the knee is going to settle or not.
Locked knees however are different and should be referred for early hospital treatment. In this situation a piece of the torn cartilage is blocking the knee from going out fully straight and this will not clear itself. Delayed treatment in this situation results in a significant increase in rehabilitation time and makes it very difficult to finally get the knee out straight. The knee of course may also be blocked by a fragment of joint surface or the torn anterior cruciate ligament stump.
Often, symptoms from a meniscal tear are related to activity and are exacerbated by sport or catching the foot on the ground, sharply twisting the knee. Patients will often describe that their knee has settled but this may be because they have generally stopped the actions that precipitate the pain.
Surgical Treatment
The main stay of surgical treatment for a torn meniscus that is causing symptoms of pain and swelling is arthroscopic resection of the torn fragment. This is usually a day case procedure with the post operative recovery taking one week to return to desk work and two weeks to manual work. Sport can be commenced after that stage.
Repair of the torn fragment, stitching it back into its normal place, is a possibility but only a small proportion of tears are of the type that can be treated by such technique. This is because the meniscus does not have its own blood supply apart from the peripheral part and tears are uncommon in this area. If repair is undertaken then a strict rehabilitation programme has to be followed limiting knee bend for the first two to three months.
Meniscal transplantation and the use of synthetic scaffolds are new options for the management of patients who are suffering after resection of whole or part of their meniscus.
Meniscal Scaffolds: Regenerating the shock absorbers in the knee
The menisci of the knee make the sockets for the thigh bone to rotate in and they provide the shock absorber for impact loads. If a substantial amount is removed after injury then this can result in early wearing of the joint surfaces. Complete loss of the meniscus usually results in early arthritis developing within 10 – 15 years.
The Meniscal Scaffold implant is a new device designed to rebuild the meniscus after part of it has been removed. This procedure of partial meniscectomy is very common and is usually successful in relieving pain. However a small proportion of patients will develop persistent pain felt in the side of the knee due to the lack of the normal thickness of the meniscus.
The implant acts as a scaffold for new tissue to grow into and regenerate the healthy cushion. Early published results show it to be successful in relieving pain after meniscectomy. However the long term benefit of reducing the severity of later arthritis in the knee is not yet fully clear as the technology has not been around long enough.
The brand of implant that we currently use to regenerate the meniscus when part of it has been removed is the ACTIFIT, supplied by Orteq. It was developed in Belgium and is made from a polyurethane polymer. Laboratory studies indicate the scaffold may still be present 5 years after implantation giving the body longer time to form a new natural regenerated meniscus.
The ACTIFIT Operation and Rehabilitation
The implant is inserted at key-hole arthroscopic surgery which is usually a day case procedure. The incision to get the implant into the joint is about 2 – 3 cm long.
Rehabilitation after surgery naturally has to be slow as the body has to grow tissue into the scaffold and this is a slow process. Full weight on the leg is allowed at 8 – 10 weeks and the specific rehabilitation program is tailored to each patient depending on the state of the knee surfaces and the amount of new meniscus inserted. Biopsy studies looking at the new tissue under the microscope have shown that the new tissue is fairly strong by 12 months. Impact sport is therefore not allowed for the first 12 months.
For more detailed information see www.orteq.co.uk
Meniscal Allograft Transplantation: for when the whole meniscus has been removed.
If the whole meniscus has been removed then the scaffold synthetic substitute will not suffice and a meniscal transplantation using a donor graft is indicated. We have now performed over 140 meniscal transplants.
Meniscal Transplantation involves implanting a donor graft (allograft) supplied from a tissue bank in the UK or from the USA. The remnants of the old meniscus are trimmed back to make a fresh bed for the new meniscus which is then inserted by keyhole surgery (arthroscopy) and stitched to the original bed. It then heals to the bed on the side capsule of the knee joint so that it can provide cushioning for the smooth articulating surfaces.
Grafts are donated rather like heart transplant donors and are very carefully prepared by the regulated tissue banks to ensure that the tissue is as free of disease risk as is possible. This process has been highly regulated and advances in testing for infections such as Hepatitis and HIV has meant that the risk of contracting severe infections through the grafting operation are now very small. Though difficult to fully quantify, the risk is less than that from a blood transfusion. Grafts are decontaminated and then cryopreserved until required.
Indications for Meniscal transplantation surgery
The procedure is indicated when there is no effective rim of meniscus remaining to support the joint surfaces. This occurs when there has been a large tear and when it was not possible for the surgeon to salvage the meniscus by repairing it. Not everyone needs a transplant but if there is progressive pain and symptoms limiting activity then the procedure may be indicated.
There is often a feeling that it is necessary to always replace the meniscus if it is removed, based on the argument that it will prevent or delay the onset of later arthritis. This is a difficult issue, but because the rehabilitation period is long and because the operation is not without risks, meniscal transplantation is usually only performed when symptoms of pain on activity begin to cause interference with your quality of life.
The quality of the result of the operation is a key factor in deciding the indications as the replacement tissue is, after all, a donor graft that may not be as strong as the original and it takes time for it to fully integrate into the knee. Having invested a year of time in getting it right after surgery the thought of going back to full contact sports such as football and rugby could be considered ill-advised!
Recent research looking at the outcome by the leading surgeons in the US and in Europe would indicate that at 10 – 13 years approximately 70% of patients still have good function and have not had further surgery. Most have been able to do light sports. The occasional professional athlete may report being able to get back to high level but it should be remembered that professional athletes may have different goals.
Following surgery the rehabilitation process involves using a knee brace for the first 6 weeks while the new meniscus heals in place but return to any form of sport is not before 6 months. Impact pivoting sports are probably best avoided.
Additional Procedures
In over 50% of our cases the transplantation operation is performed in conjunction with other procedures and depending on this the rehabilitation regime may change. Additional procedures may include
- Surgical procedures to repair the joint surface such as microfracture or autologous chondrocyte implantation
- If the joint is failing because the leg is out of alignment (bow-legged or knock-kneed) then osteotomy or realignment corrective surgery is needed.
- If the knee is unstable due to a ligament injury then transplantation can be combined with anterior cruciate or posterior cruciate ligament reconstruction.
Overall meniscal transplant is an exciting option for the damaged knee allowing for substantial improvement in the quality of your life. Though a challenging procedure with a long rehabilitation program, the technique alone or when combined with other surgery, provides a realistic biological option for knees, hopefully avoiding, or at least delaying, the need for metal and plastic knee replacement operations.
Patello-Femoral Problems
A synopsis of diagnosis and management
The patello femoral compartment of the knee is a common source of pain and symptoms in the knee. The aim of this section is to provide a simple guide and outline for the diagnosis and management of patients presenting with anterior knee pain.
In general pain can be thought of as an emerging from the patello femoral joint in the patients who describe that it is their “knee that hurts”. This means that when a patient presents complaining of pain alone then the aim of questioning is to determine whether the source is the medial compartment (indicating a meniscal or degenerative problem), lateral compartment, again indicating meniscal or degenerative problem, or the patello femoral structures and anterior compartment. When patients state it is their “knee” that hurts they usually grasp the front part of the knee indicating the anterior compartment rather than pointing with a finger to the medial or lateral compartments specifically.
Overview of Patello Femoral Problems
The following classification and description of patello femoral problems is given as a guide for a decision making in anterior knee pain problems.
Classification:
Essentially this categorisation is dividing patients into those with a potential for patella dislocation, defined as potential patella instability, those who have had clear episodes of dislocation and those patients with normal anatomical alignment producing the subcategory of “painful patella syndrome”. This subcategory can be further subdivided as follows.
Painful Patella Syndrome:
In order to lead to a conclusion for which subcategory of patient fits in, the following three questions need to be considered when assessing a patient presenting with anterior knee pain or patellofemoral problems.
Three Questions for Patello Femoral Problems:
Is there mal-alignment?
Is the problem in the peri-patella tissues?
Is this simple overload?
Mal-alignment
Mal-alignment is the term used in the assessment of patello femoral problems indicating that the patella is not sitting in its proper place and the joint surface and tissues are therefore under abnormal load. There is clearly a spectrum of mal-alignment problems: from true dislocation at one end of a spectrum, where the patella is pulled off to one side, and mild mal tracking, where the patella does not track centrally in the trochlea groove at the end of the femur where it is meant to sit.
The mainstay of diagnosis is therefore directed at excluding or detecting abnormalities of alignment and tracking of the patella (see later).
The Peri-patella Tissues
There are various specific causes of anterior knee pain and patello femoral problems that are related to the tissue around the knee. These are isolated diagnoses and are summarised as follows:
- Patella tendonitis: otherwise known as jumper’s knee and characterised by pain and tenderness at the lower pole of the patella (junction of the patella tendon and bone). Diagnosis is made by finding localised tenderness at that site.
- Medial plica pain: pain localised on the medial aspect of the knee in the region of a cord-like band extending from medial patella to medial femoral epicondyle with localised tenderness.
- Neuroma: isolated tender trigger point with radiating electric shock type pain characteristic of a neuroma.
- Bursitis: inflammation of the pre patella or infra patella bursa.
- Tibial tubercle problems: prominent tibial tubercle from childhood Osgood Schlatter.
Overload problems: what is the source of pain
Articular cartilage itself does not have any pain fibres and pain seems to originate from either the subchondral bone or the soft tissue surrounding the knee, which is densely innovated. A likely theory is that overload on the patello femoral joint results in an increase in pressure in the subchondral bone and leads to the sensation of pain. This explains the treatment rational for reducing overload on the patello femoral joint and thereby reducing pain.
Remember other causes of knee pain.
It is important not to remain too focused on the knee as a source of pain. We must not forget that knee pain may be felt from radicular origin (spine) and the hip (childhood conditions of Perthes and SUFE plus adult problems of hip OA).
Obtaining clues from description and history
Pain: most patients report anterior knee pain which is typically activity related and tends to be worse on climbing or descending stairs. Symptoms in the athlete are exaggerated after running over hilly ground. Symptoms are classically worse when sitting with the knee bent for prolonged periods such as in a cinema or car.
Instability and giving way: patients describing this symptom are likely to have problems with true patella dislocation or recurrent subluxation (patella seeming to slide laterally during a twisting movement). This needs to be differentiated from the buckling of the knee on pivoting associated with ACL rupture. Subluxation is virtually always lateral due to the pull of the quadriceps muscle.
Mechanism of injury: a direct blow to the anterior part of the knee such as falling on a concrete step will tend to result in traumatic anterior knee pain and impact damage on the articular cartilage of the patella or the corresponding trochlea surface. Landing on the anterior tibia may drive the tibia posteriorly, causing an injury to the posterior cruciate ligament resulting in the tibia sagging and overloading the patello femoral joint.
Insidious onset of symptoms: this usually indicates that there may be an anatomic pre-disposition to anterior knee pain or specific training activities may have caused an overuse problem and this may be well recognised and treated with retraining
Examination
The key features on examination: examination should confirm that the pain is originating from the patello femoral compartment of the knee and as such this will involve attempts to reproduce the symptoms. The main aims of examination are therefore:
- Reproduction of symptoms.
- Evaluation of the alignment.
- Assessment of knee flexibility.
- Location of painful structures.
Assessment to answer the question: is there mal-alignment?
The simple quick key steps to assessing mal-alignment are:
1 Standing alignment (bare foot).
- Valgus angle: angle between quadriceps pole and patella tendon – greater than 25° in females and 20° in males.
- Rotational abnormality (squinting patella – patellae pointing inwards with the feet facing forwards).
- Excessive pronation of the feet (flat feet).
2 Assessment while sitting.
- Tubercle Sulcus angle greater than 10°. Tibial tubercle should appear directly below the patella. Angle greater than 10° indicates significant lateral pull on patella.
- Patella tracking on extension – detection of subluxation of patella as the knee approaches full extension.
- Patello femoral crepitus – painful grating sensation on extending the leg against gravity noticed on palpation of the joint.
3 Supine assessment of patella mobility.
- Sideways mobility of patella – medial glide of ¼ or less of the patella width suggests abnormally tight lateral retinaculum.
- Patella tilt – patella should be in the same plane as the bed with the feet pointing anteriorly: a downward lateral tilt indicates tight lateral structures.
- Patella apprehension – reluctance to allow lateral push on the patella.
- 4 Assessment of other joints and general tightness.
- Hip rotation at 90° – should be symmetrical and pain free.
- Straight leg raising – exclude sciatica radiation of pain down the back of the leg.
- Tight hamstrings causing anterior knee pain – straight leg raising reproduces anterior knee pain rather than sciatica.
5 Tender points.
- Patella tendinitis – tenderness at junction lower pole patella and patella tendon.
- Medial plica – tender over the band between patella and medial epicondyle.
- Patello femoral irritation – compression of patella on articulation at varous stages of flexion to reproduce pain.
6 Other tests.
Other subtle tests can be performed looking for tightness of structures. These could include assessment of quadriceps flexibility by lying the patient prone and assessing the ease the knee bends heel to bottom. Iliotibial band flexibility is assessed by Obers test. The detail of this is outside the scope of this section.
Management overview
The examination detailed above combined with use of the classification at the beginning of this section will lead to various management options.
1 Objective patella instability.
In this scenario patients have sustained true patella dislocation, often on several occasions and it would be expected to find abnormal anatomy with poor patella tracking.
Management: patients should be referred for orthopaedic opinion as they are likely to need corrective surgery for the misalignment. A rehabilitation programme should be commenced. It would be essential to try at least 2 – 3 months of appropriate rehabilitation before undergoing surgery.
2 Potential patella instability.
In this situation the patella may never have fully dislocated but the patient may experience symptoms of the patella jumping or sliding nearly out and distrust in the knee. It is usual then to find signs of abnormal alignment.
Management: referral for physiotherapy rehabilitation programme which would commonly involve taping and probably the use of a patella supportive brace. Referral for orthopaedic opinion could be delayed awaiting outcome of rehabilitation which stands a high chance of helping. Persistent subluxation symptoms are however bad and raise the chance of later degenerative change. Early surgical correction is far preferable to late osteoarthritis.
3 Painful patella syndrome.
In this situation there will be normal anatomical alignment and the patient will generally complain of anterior knee pain localised to the patello femoral compartment area.
Management: this depends on the underlying diagnosis.
4 Primary painful patella syndrome.
When this occurs in the teenage female then a conservative approach with physiotherapy is best adopted with procrastination, avoiding the temptation for surgery.
5 Overused knee.
This is diagnosed when there are no obvious anatomical abnormalities and there has been some activity that has prompted overuse of the knee. Again a rehabilitation programme would be directed at detecting and altering the precipitating factor.
6 Secondary problems
- Medial plica: this can be partly treated with physiotherapy but often needs surgery to remove it.
- Detection of PCL laxity: This is likely to need orthopaedic referral and a PCL brace may be indicated, prescribed by the hospital.
- Post traumatic anterior knee pain. This occurs following a direct blow to the anterior part of the knee, impacting the patella on the femoral groove. Rehabilitation is a first line of treatment but if symptoms persist beyond a year then arthroscopy may be indicated, hence referral to orthopaedic surgery at that stage.
- Patella tendinitis. Localised pain at the lower pole of the patella is best treated with physiotherapy and a specific ‘eccentric exercise’ programme. Referral to orthopaedics is indicated if symptoms have persisted for three months.
Background information on rehabilitation options for treatment
As would be noted from the management overviews outlined above, patello-femoral rehabilitation is a key part to treatment of these problems. Specialist physiotherapists with an interest in this area are key to the management and certainly aid in the diagnosis of these problems. Multiple treatment modalities are available including an exercise programme, soft tissue stretching and pain management. The use of biofeedback principles, orthoses and analgesics are also very important.
Specific programmes of exercise vary between practitioners, but are likely to include:
- Stretching of the hamstrings
- Stretching of the hips
- Strengthening of hip external rotation
- Strengthening of the vasti muscles, including controlled step-down exercises
In general, closed kinetic chain knee extension exercises, with the foot on the ground – are preferred. These are in preference to open chain exercises as excessive patello femoral joint forces can be generated when the foot is not in contact with the ground. Eccentric exercises are especially important for specific areas of tendinitis.
Patella taping is also a key element to rehabilitation and physiotherapy. In this method taping is applied to the patella to re-direct the tracking and therefore reduced pain. Patients can be taught how to apply taping themselves. The principle is that once symptoms are under control the taping can be discontinued. At this stage, the patient’s own muscle balance has returned to control patella tracking and overload. It should be stressed to patients that taping on its own is unlikely to be effective – it must be combined with stretching and strengthening as outlined above.
Further details on these aspects can be obtained from the rehabilitation department.
Background Information on Surgical Options for treatment
This section looks at the potential surgical treatments that are employed for patello-femoral problems and outlines the scope of the treatment modalities.
1 Arthroscopy.
Arthroscopy is generally not the first line treatment or investigation for patello-femoral problems. It becomes indicated if there are mechanical symptoms and signs affecting the joint. Options for treatment using the arthroscope include:
- Debridement and shaving of roughened articular surface.
- Release of tight adhesions within the knee.
- Release of tight lateral capsule and retinaculum in the presence of lateral tracking of the patello-femoral joint when viewed with the arthroscope. (Lateral release procedure).
More information on arthroscopy can be found in Appendix A.
2 Medial Patello-Femoral ligament (MPFL) reconstruction.
Over the last fifteen years or so, the importance of the medial patellofemoral ligament (MPFL) as the primary soft-tissue restraint to lateral displacement of the patella has become recognised. Rather than being a distinct ligament – such as the anterior cruciate ligament – it is formed by a concentration of fibres of the joint capsule. It is most active over the first 30 degrees of flexion, beyond which the trochlea groove is engaged by the patella.
The MPFL can be ruptured following lateral dislocation of the patella. Where the bony anatomy is relatively normal then rebuilding the MPFL is the procedure of choice to stabilise the patella.
In the most commonly-employed surgical procedure, the gracilis tendon is first harvested as a single graft. It is then used to recreate the tension between the medial border of the patella and the attachment of the MPFL to the medial epicondyle of the femur. Proper anatomical positioning of the graft is crucial to the surgical outcomes. Cases of medial subluxation, medial articular overload and recurrent lateral instability have all been reported as a result of improper surgical technique.
3 Bony re-alignment of distal structures.
This option involves transposing the tibial tubercle towards the medial and anterior direction depending on the type of misalignment. The effect of this is to reduce the lateral pull on the patella by the quadriceps.
These procedures are less commonly performed since the advent of MPFL reconstruction but the main types of osteotomy performed include:
- • Fulkerson osteotomy: this shifts the tibial tubercle and therefore patella tendon medial and anteriorly through an oblique osteotomy held in place with two screws.
- • Distal and medial transposition tibial tubercle. This is used when the patella is riding high (patella alta) in the trochlea groove leading to potential instability. Shifting the tubercle distally brings the patella into a more located position within the trochlea groove.
These surgical procedures require the use of a protected range of movement brace after surgery, for four to six weeks as the bone heals, followed by a two to three months rehabilitation programme.
4 Trochleoplasty
One of the causes of an unstable patella is trochlear dysplasia, meaning that the trochlear groove of the femur is too shallow or uneven. One option for dealing with this is to aim to reshape the anatomy of the trochlea surgically. Various options are available, including deepening the groove, or raising the lateral wall, depending on the specific problem. This is usually an open operation.
